Because Home Care is the BEST Care!
Blog Layout
Seniors and Vision
September 22, 2022
Seniors with Vision Loss and How Caregivers Can Help
Seniors are prone to eye disorders, so exams are crucial. Problems develop painlessly and have no symptoms and individuals may not notice changes in their vision.
Seniors and Vision Loss: How to Adapt to Changes in Sight
The importance of sight exams
Annual eye exams help seniors keep regular tabs on their eye and overall health. Eye exams can also uncover other potential health problems such as artery blockages, hypertension, high cholesterol and diabetes.
(www.vsp.com)
How Loss of Sight Impacts Driving
Age-related vision changes that affect seniors’ ability to drive:
According to the U.S. Centers for Disease Control and Prevention, 2.8 million seniors are thought to have severe vision impairment – defined as either blindness or difficulty seeing, even with eyeglasses.
How loss of sight impacts hygiene
Help prevent falls when caring for someone who has low vision or blindness:
Home Care Tips:
Point out obstacles in their home to them or family members that may be potential hazards, such as a throw rug or cables on the floor, which could cause them to trip and fall.
Seniors and Vision Loss: How to Adapt to Changes in Sight
The importance of sight exams
Getting an annual eye exam is important for people of all ages, but especially for older individuals. Senior citizens are more prone to eye disorders such as glaucoma, cataracts and macular degeneration than younger people. Early detection is critical with these three diseases.
Age-related eye problems can develop painlessly and have no early symptoms. Individuals may not even experience changes in their vision until the condition has become more advanced.
(www.vsp.com)
How Loss of Sight Impacts Driving
Age-related vision changes and eye diseases can negatively affect driving abilities even before an individual notices any symptoms.
- Not being able to clearly see road signs
- Difficulty seeing objects up close, like the car instrument panel or road maps
- Difficulty judging distances and speed
- Changes in color perception
- Problems seeing at night or in low light
- Difficulty adapting to bright sunlight or glare from headlights
- Experiencing a loss of side vision
According to the U.S. Centers for Disease Control and Prevention, 2.8 million seniors are thought to have severe vision impairment – defined as either blindness or difficulty seeing, even with eyeglasses.
How loss of sight impacts hygiene
- Loss of vision can impact all areas of one’s life including day-to-day activities and personal hygiene. There are things caregivers can do to help seniors who have experienced vision loss.
- Mark their toothbrush with a tactile or contrasting-colored tag so it’s easily distinguishable.
- Move hygiene products to pump packs that squeeze out pre-measured amounts.
- Put shampoo and conditioner in different colored or shaped bottles so they are easy to identify.
How loss of sight can be dangerous
Vision loss can be dangerous for seniors and can affect other areas of their life. The CDC estimates that about 1.3 million older, vision-challenged Americans fell at least once in 2014. Since falling is among the leading injuries that sends seniors to the hospital, preventing falls is critical. Help prevent falls when caring for someone who has low vision or blindness:
- Leave things are you found it in their home. If something has to be moved, tell them where you have moved it.
- Be careful when cleaning the house. Cords, wet floors and a mop and bucket are all potential hazards they could trip or slip over.
- Shut doors completely or leave them fully open. A half-open door is a hazard.
- Replace light bulbs to provide them with good lighting in all the rooms, staircases, closets and hallways.
- Declutter their home and help them dispose or items that are no longer meaningful or necessary.
- Have grab bars installed in stairways and bathrooms.
Home Care Tips:
Point out obstacles in their home to them or family members that may be potential hazards, such as a throw rug or cables on the floor, which could cause them to trip and fall.

By Hibu Websites
•
April 3, 2025
We all know the feelings and memories that different songs evoke - a song that harkens to our first love, reminds us of happy times in our childhood, that our parents use to play in the early evenings, that we used to sing with our friends. Out loved ones have these same memories tucked away too. And there is some evidence that these memories are easier for them to retrieve than names or faces. Current research indicates that the areas of the brain that store musical memories are relatively unaffected by Alzheimer's, dementia, and Parkinson's. Even playing an instrument is tucked away in a part of the brain that can remain untouched by their ailment. Some studies have reported that listening to music can even bridge the gap for a recall of specific memories. In non-demented Parkinson's disease, music can lead to more fluid motor flow, such as dancing. The emotional experience of listening to music can increase the release of dopamine, which is a brain chemical lacking in those with Parkinson's disease. Unfortunately, this improvement stops the moment the music does. For dementia patients, the benefit of music can improve mood, behavior, and cognitive function far beyond when the music stops. Healthy adults who are leaning to play an instrument show improved performance on some cognitive tests. While playing music, multiple areas of the brain are activated and, in the long run, this can help reconnect the two sides of the brain. Perhaps it is never too early for all of us to start using music to help prevent cognitive decline. ( Practical Neurology , The Michael J. Fox Foundation , and Mayo Clinic ) Playing Music Playing music is a complex undertaking that engages multiple areas of the brain simultaneously, helping to improve brain health or, at a minimum, to slow decline. Playing an instrument requires: Fine motor movements and an intact sensory system to manipulate an instrument Immediate processing of visual and auditory elements of a melody Mathematical precision and internal rhythm to keep tempo Emotional interpretation of the sound Coordination with other performers ( The Michael J. Fox Foundation ) What you Can Do at Home While specific goals should be guided by a licensed Music Therapist, there is certainly a benefit to providing your loved one a musical outlet. Consider creating playlist they can use to sing along or tap their feet. If they used to play an instrument, perhaps giving them access will spark old memories. Combing songs with daily routine makes necessary activities like eating and washing easier. The practice develops a rhythm that helps recall memory of the activity, empowering someone whose body and mind needs all the help it can get. Listen to the music with your senior, especially at first. Look for clues in their facial gestures and body language to gauge the effect the song is having on their mood. Music can be stimulating or soothing. It can conjure a range of emotions from elation and joy to melancholy and irritation. Music can turn a bad mood around, trigger lost memories, and ground people to the present moment. If you feel a song or playlist is having an adverse effect, remove it from the playlist. Choosing Music Look at the top pop songs from the years when your loved one was between 18 and 25. Experts say that this is when we hone our musical tastes. Certified musical therapist Rachel Rambach created a list called 12 Songs Every Music Therapist Should Know that might be good jumping off point to start your own list. Songs on her list include Over the Rainbow, You Are My Sunshine, and Amazing Grace. Even songs like Take Me Out to the Ballgame can inspire positive memories. As you're considering adding music to help a loved one who has Alzheimer's disease, consider these tips: Think about their preferences. Ask them directly or gauge their reactions to a range of music. Involve family and friends by asking them to suggest songs or make playlists. Set the mood. To calm your love one during mealtime, sundown, or a morning hygiene routine, play music or sing a song that's soothing. To boost your love one's mood or help them get moving, use more upbeat music. Avoid over stimulation. When playing music, eliminate competing noises . Turn off the TV. Shut the door. Opt for music that isn't interrupted by commercials, which can cause confusion. Encourage movement. Help your loved one to clap along or tap his or her feet to the beat. If possible, consider dancing with your loved one. Pay attention to your loved one's response. If you loved one seems to enjoy particular songs, play them often. If your loved one reacts negatively to a song or type of music, choose something else. ( Pace for Mom , Mayo Clinic , and Dementia Care Central )
By Hibu Websites
•
March 20, 2025
Preparing seniors for doctor visits Getting to a doctor visit, as well as understanding and implementing medical advice, can be a challenge for seniors. Aging involves changes in health, physical ability, and medical risks. On average, older adults in the US tend to be in a healthcare setting about 17 days a year. Given how common (and often necessary) it is for seniors to interact with doctors, it is important to help seniors navigate doctor visits well. A start to finish doctor visit checklist For seniors, doctor’s visits are stressful. Use this checklist to help ease anxiety * Arrange transportation to and from the appointment * Identify whether or not a companion is necessary for the visit * Check if the appointment or associated tests require seniors to contact their insurance company ahead of time for pre-certification or other purposes * Pack everything needed for a successful appointment Insurance card Photo ID Payment for co-pays or other charges Contact information for other doctors List of current medications List of allergies/medical conditions Medical records, if needed A list of questions for the doctor And notepad or device for note-taking *Verify at checkout after the appointment If further testing or labs required When new prescriptions should be picked up If there are instructions or treatment notes seniors can take home with them When follow-up appointments are scheduled If any payment is due How to Help Seniors Advocate for Themselves Often, seniors feel nervous or powerless when in healthcare settings. Encourage seniors to attend their appointments confidently and to speak up for themselves. Remind seniors to: Bring glasses or hearing aids if necessary to support effective communication Prepare to share what has been going on in their lives and to ask questions Ask for directions, diagnoses, and notes about the appointment in writing Get a second opinion if they are uncomfortable or unsure of something a doctor says Take a family member or close friend for support if self-advocacy is challenging for them Tips to see the Doctor Less Often Following doctor's instruction and taking care of oneself are great ways for seniors to reduce the number of appointments they attend. There are also alternatives to traditional doctor visits that seniors can benefit from such as: Web-based medical services Virtual or over-the-phone appointments Retail clinics, especially for flu shots or common, minor illnesses Urgent care centers Cyclical Reasons Seniors Should See the Doctor One of the reasons aging adults tend to see doctors often is for cyclical treatments, check-ups, or preventative care. For instance, seniors should plan on: Annual check-ups A colonoscopy every decade Annual vaccinations Regular eye exams Dental exams twice a year Screening for cancer, thyroid disorder, etc. Home Care Tip Help seniors who are active online to understand that the web does not have a medical degree. While medical information could be helpful to reference and understand more about health, only professionals with education and training should make a diagnosis and prescribe treatments.
By Hibu Websites
•
March 6, 2025
How to Spot Symptoms of Mental Illness in the Elderly Normal signs of aging can mask symptoms of mental illness in the elderly. About 58% of people over the age 65 think that depression is a normal part of aging. Myths like this often prevent seniors from having mental illnesses identified and treated. ( Mental Health America Survey ) According to the CDC ( cdc.gov ), an estimated 20% of people over the age of 55 have a mental health issue. Many mental illnesses can significantly affect physical and social well-being. Mental illnesses can, however be hard to distinguish from regular signs of aging. 8 Common Symptoms of Mental Illness in the Aging Signs of mental illness in the aging may be expressed verbally in discussion. Often, though, the elderly exhibit their symptoms behaviorally or physically instead. Look for these 8 symptoms in the elderly to spot mental illnesses during the aging process. 1. Unusual Avoidances For seniors, avoiding extreme heat or exhausting activities makes sense. However, avoiding eye contact, using the bathroom, touching certain objects, or participating in events is atypical. Watch for extreme or unusual avoidances. 2. Difficulty Making Basic Decisions Decision-making is affected by memory, emotions, and judgment processes. When seniors struggle to make basic decisions or change their minds frequently the issue may be cause by mental illness. 3. Unexplained Stomach Distress A person’s gut reveals much about their physiological state. If a senior has unexplained digestive problems, they may be experiencing feelings or thoughts due to mental illness that are causing distress. 4. Agitation or Moodiness Irritability among seniors may occur as a result of physical conditions like chronic pain. However, agitation and moodiness that is disassociated from a reasonable cause can indicate a mental health problem. 5. Change in Appetite or Sleeping Patterns Often a change in eating or sleeping habits is the first sign people notice of depression. Pay attention to a senior’s routine and ask questions to understand why their habits may otherwise be changing. 6. Disinterest with Fatigue Feeling tired can occur as a result of aging. When tiredness becomes constant or chronic fatigue, it may be a sign of something more. Be on alert for a disinterest in hobbies or decrease in socialization due to fatigue. 7. Hallucinations or Delusions If a senior recalls information that doesn’t make sense or that never occurred, they may be experiencing hallucinations or delusions. These symptoms may present as paranoia or as simple confusion. 8. Sudden Changes in Behavior and Attitude It is unusual for optimistic seniors to suddenly feel sad all of the time with no cause. Likewise, a senior who participates in a hobby regularly and without explanation stops, may be struggling with a mental illness. ( Todays Geriatric Medicine ) Common Mental Illnesses Among Seniors Depression Anxiety Memory Diseases Cognitive Impairment BiPolar Disorder ( cdc.gov ) Pre-existing conditions such as: Dementia Alzheimer’s Parkinson’s Stroke Diabetes Thyroid disorders Degenerative diseases Significant Life Changes Like: The loss of a loved one Moving Becoming disabled Enduring an illness or injury New medications ( Helpguide ) Home Care Tip: Due to stigmas and myths about mental illness, many seniors are unwilling o visit a mental health professional like a psychologist. Seniors are often more likely to be honest with primary care providers and may receive treatment from them more willingly.

By Hibu Websites
•
February 20, 2025
Our minds are powerful tools for creating health and wellness. While studies haven't identified precisely why positive popel are healthier, researchers suspect that it is because people who are more positive process stress better and move through hard situations more easily. Negative attitudes and feelings of helplessness can create chronic stress, which can, in turn, damage the immune system. Anger and hostility are related to health conditions such as high blood pressure, cardiovascular disease, digestive disorders, and increased instances of infection. Surprisingly, the tendency toward a positive or negative outlook does have a genetic component. However, this doesn't mean that people can't improve their outlooks. Some tips to improve your outlook include: * Smile more. Even fake smiling can reduce heart rate and blood pressure during stressful situations. * Practice reframing. Instead of stressing about a current situation, try to find a positive aspect to it. * Build resiliency. Having friends and family nearby to share the situation with, accepting that change is a part of life and finding new wyas to adapt, and feeling like you have the control to change the current situation are all ways to embrace whatever life throws your way. * Share your feelings. Often, we spend too much time in our heads. Sharing our feelings with a trusted other can help find a different way to look at a situation. If others are mired in their current negative situations, encourage them to share their fears. ( Johns Hopkins Medicine , University of Minnesota , and University of Wisconsin Health ) While loved ones might resist the idea of optimistic thinking, there are health reasons to ask them to reconsider. Positive thinking can lead to : *Better sleep * Increased life span * Lower levels of distress * Lower rates of depression * Greater resistance to the common cold * Better cardiovascular health * Better coping skills during extreme hardship Tips for Creating a More Positive Outlook * Get better sleep * Take a walk outside * Follow a healthy lifestyle * Practice positive self-talk * Surround yourself with positive people * Be open to humor or create a place for smiling and laughing every day * Consciously work on experiencing three positive emotions for every negative one. * Actively evaluate your self-talk at various points during the day to see how you're doing. ( Mayo Clinic and University of Wisconsin Health ) Are you a negative or positive thinker? Listen to your own self-talk -- that endless stream of unspoken thoughts that goes through your head. Some forms of negative self-talk to watch out for include: Filtering - This means magnifying the negative aspects of a situation and not acknowledging the positive. For example: Your loved one had a good night's sleep, a fun phone call with their grandchild, and took a walk on a beautifully sunny day outside. But then they tripped and fell with minor injuries. At the end of the day, did they say it was a "bad" day because of the fall or a "good" day because of the rest? Personalizing - When something bad occurs, you or your loved one automatically takes the blame. Sometimes no one is to blame. Catastrophizing - You or your loved one uses language that makes things out to be much worse than they are, or assumes that because one bad thing happened, it's all downhill from there. Single events in the day are rarely the "worse" or "most horrific. " Polarizing - You or your loved one sees things as either good or bad and not the huge gray area in the middle. This leads to feeling like one is only perfect or a failure, healthy or dying tomorrow, capable or completely incapacitated. If you are seeing these tendencies in your loved one, you should take care to address the subject, as they are more likely to see it as an attack and apply all of the above thought processes to that interaction. ( Mayo Clinic ) Positive Self-Talk * Affirm daily what is good about you. * Remove the words "never" and "always." * Express gratitude -- either aloud or in your head. * If you make a mistake, take a moment to forgive yourself. * Don't say anything to yourself that you wouldn't say to someone else. ( Mayo Clinic )

By Hibu Websites
•
February 6, 2025
Asthma is often characterized by coughing, wheezing, shortness of breath, and chest tightness or pressure. According to the CDC, 1 in 13 people suffers from asthma. It is characterized by the inflammation of the bronchial tubes in your lungs with increased production of mucus. This causes less air to be taken in, with less oxygen to be distributed throughout the body. Asthma can be hereditary, so it is beneficial to know family health history. It is also connected to other allergic conditions like atopic dermatitis or hay fever. If your loved one is prone to allergic reactions and begins to have trouble breathing, have a doctor determine if they have developed asthma as well. Asthma is more commonly seen in adults with occupations that subject them to airborne chemicals, such as those used in farming, salon work, or manufacturing. ( University of Rochester Medical Center ) How to Control Asthma Prescription drugs Monitor lung capacity with regular doctor visits Use a Peak Flow Meter at home Develop an asthma action plan with your doctor Use a rescue inhaler or nebulizer when necessary Stop smoking and vaping Exercise regularly to maintain a healthy weight and help with breathing ( Cleveland Clinic ) Common Asthma Triggers Airborne allergens, such as pollen, dust mites, mold spores, pet dander, or bug waste Respiratory infections, including the common cold Physical activity Cold Air Air pollutants, such as smog and smoke Some medications including beta blockers, aspirin, ibuprofen, and naproxen sodium Strong emotions or stress Sulfites Gastroesophageal reflux disease (GERD) ( Mayo Clinic ) Asthma Attacks While they may generally have trouble breathing, people who suffer from asthma are most concerned with preventing an attack, a sudden onset of severe symptoms. Early signs of an attack include: Frequent cough, especially at night Losing their breath easily or shortness of breath Feeling very tired or weak when exercising Wheezing or coughing after exercise Feeling tired, easily upset, grouchy, or moody Signs of a cold or allergies (sneezing, runny nose, cough, nasal congestion, sore throat, and headache) Trouble sleeping If your loved one has an asthma action plan, generally including an inhaler and breathing treatments, it is critical to intervene during these early symptoms. If you notice that the inhaler is needed multiple times a day or becomes a challenge for your loved one, talk with the doctor about alternatives such as a nebulizer or oral medications. The attack can also include some or all of the following: Severe wheezing when breathing both in and out Very rapid breathing Chest pain or pressure Tightened neck and chest muscles, called retractions Coughing that won't stop Difficulty talking Feelings of anxiety or panic Pale, sweaty face Blue lips or fingernails Gradually, the lungs will tighten so there is not enough air movement to produce wheezing. It is at this point that hospital intervention is critical. Some people interpret the disappearance of wheezing as a sign of improvement and fail to get prompt emergency care. ( WebMD and Asthma and Allergy Foundation of America ) Who Does Asthma Affect? Asthma can affect children and adults. Symptoms are typically more intermittent in children and persistent in adults. Unfortunately, adult-onset asthma has a higher death rate than childhood asthma. This is perhaps because symptoms are ignored by the adult or their caretakers and attributed to weight or just a regular part of getting older. Do not ignore wheezing or coughing, especially if it seems chronic. It is important to seek medical advice to ensure that shortness of breath is not something more serious. Some of the factors that might increase the risk of adult-onset asthma may include: Being overweight Pregnancy or menopause A buildup of allergens such as cats, cigarette smoke, chemicals, mold, or dust Childhood asthma will often go into remission for a decade or so then return in a person's 30s or 40s. Remember that asthma does not have a cure. It is important to maintain the medical relationships and awareness throughout your lifetime. ( Cleveland Clinic )

By Hibu Websites
•
January 23, 2025
We all know how difficult it can be to keep track of doctor recommendations, medications, advice, insurance, and costs when we’re dealing with our own medical care. Compound that with the confusion of dementia or reduced short term memory, and a decrease ability to communicate their needs and challenges, and the process for your senior becomes even more daunting. Your loved one depends on someone to help keep the big picture straight. How can you be an effective advocate for your loved one? Most importantly, you need to care. When you care about their health and general well-being, you are more inclined to ask the deeper questions, seek out additional opinions, research other approaches, and push back on unnecessary expenses. Other helpful traits to have are good organizational skills, some free time, physical aptitude to bring your senior to and from multiple appointments, and social skills to work with the various health professionals who are collaborating on y our seniors care plan. ( Johns Hopkins Medicine ) Health advocates, whether they are paid professionals, free placements, or family members, provide several services: Coordinate with Medicaid, Medicare, and insurance companies Help get the patient to doctor visits, testing, and procedures Track prescriptions and help ensure they take proper amounts at correct times Research alternative therapies and treatments and discuss options with the senior and their medical team Make sure that things like Power of Attorney and Living Wills are in place ( Love to Know and Institute on Aging ) Paid advocates can provide the following additional help: A complete assessment with care recommendations (usually completed in the senior’s home) Assistance finding appropriate housing and transitioning to the new living environment such as an assisted living facility Reviewing all bills from medical professionals, hospitals, and insurance companies for accuracy Identifying and securing community services such as Meals on Wheels, adult daycare, or wheelchair transportation services Handling paperwork to ensure service delivery ( Love to Know and Institute on Aging ) If you are unable to hire professional advocacy assistance, many times local senior centers can help. Often, they are familiar with resources and are committed to helping your senior maintain some level of independence. Senior centers administer a range of programs such as congregate meals, transportation services, and community education. ( National Council on Aging ) In addition, they will need the daily personal health advocacy provided by checking in on their routine, health, weight and mobility, and prescriptions. You are an extension of your senior’s mind and spirit, and will be able to be a better advocate for their health when in the doctor’s office or at the pharmacy. Even if you are working with a professional advocate, you will be able to share this information. One of the most important ways to advocate for your senior daily is helping with medication. Keep an eye out for these deterrents to taking their medications appropriately: Memory: Brainstorm creative ways that will help them remember to take the medications - alarms, notes, or pill boxes. Vision: Sometimes they simply can't see well enough to read the correct dosing. Ask the pharmacist to print the labels in large print. Hearing: They may not want to admit that they can't hear the instructions that pharmacist or doctor is giving them. Be their ears. Dexterity: Can they open the bottles easily and are the pills pre-split? Do they need your help administering eye drops or inhaled medications? Swallowing: If your loved one has difficulty swallowing, follow up with their medical team to determine if there is a liquid, patch, or other form of dosing that can be used. ( Family Caregiver Alliance ) What is a Professional Health Advocate? They are often individuals with higher degree in nursing, social work, or gerontology that help seniors with a variety of issues, including those related to medical, financial, and insurance problems. They may work out of an office, but will usually make home or facility visits. The best ones are kind, knowledgeable, and results-driven when it comes to getting your senior’s needs met. ( Institute on Aging ) Questions for the Medical Team about Medications and Treatment How will I know that the treatment is working? What are the potential side effects? How will this medicine interact with other medications that my loved one is taking? What is the cost of the medicine or treatment prescribed? Are there less expensive alternatives? Do you have written information about the treatment that we can take home? ( Family Caregiver Alliance )
By Hibu Websites
•
January 9, 2025
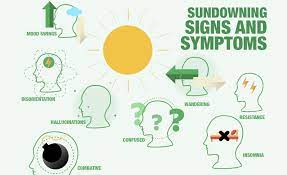
Up to 20% of adults with Alzheimer’s experience Sundowners Syndrome. Unfortunately, the exact cause isn’t known and there is no way to predict whether your senior will be affected by it. While the cause isn’t known, there are several avoidable factors that are known to aggravate it. Fatigue Shadows Low lighting A change in schedule While your loved one may act aggressive, combative, and angry, it’s important to remember that, for many of our seniors, these emotions are based in a fear response and/or an intense feeling of needing to get away. It’s not a rational set of reactions but the emotions are real to them. Your empathy is key towards driving efforts to calm and reassure them, and can go a long way toward helping control your own frustrated reactions during this time. Neither of you asked for this. Sundowning doesn’t reliably respond to medications or medical interventions. Many of the medications that might be tried have side effects that trigger alternate confusion or aggravation for your loved one. And, what triggers them now may not be what triggers or exacerbates it in the future. Sundowners or Delirium? The symptoms of Sundowners and Delirium are similar; however, they are very different conditions. Delirium often begins suddenly and doesn’t necessarily occur at specific times. Sundowners creeps up as dementia progresses and very often is more pronounced in the afternoon and evening. Some causes for delirium include: Urinary tract infection Stroke Low Blood Sugar Drug interactions Head Injury Carbon monoxide Lung or heart problems Since delirium is often a reaction to a condition, it can be more easily addressed directly and medically. ( Medical News Today ) You can help to reduce the challenges of sundowning through a multitude of holistic means: Maintain a predictable schedule, especially in the afternoon and evening. Increase the amount of daylight that your loved one is exposed to. Limit afternoon naps. Limit caffeine, sugar, and liquid during the late afternoon. Close curtains and turn on lights at sundown. Reduce the amount of activity, including TV, at night. If their confusion starts at the time of day that people are getting home from work and preparing dinner, try to decrease the chaos or move them to a quieter part of the house. Play soothing music or nature sounds. Take an evening walk. Utilize a night light in the room where they sleep. Avoid restraining your loved one or arguing with them when they are agitated. Pacing can help them work off the agitation. Reassurance, rather than argument, will help calm them. Sometimes the best solution is distraction. Offer your senior a favorite snack, beloved object, or change in activity. Even simple tasks like folding laundry can be used to distract and involve their brain in a less reactive way. Since Sundowner’s does not always follow a predictable pattern, it is important to pay attention to potential triggers, as well as to which activities seem to soothe the confusion. Knowing your loved one’s triggers can potentially help you gift them with the internal tools to handle their own feelings of frustration and confusion. ( Mayo Clinic , Alzheimer’s Association , AARP , and Medical News Today ) The Calming Properties of Aroma and Touch Therapy Many institutions have successfully incorporated aroma and touch therapies into their evening routines. You can employ this in your home as well. A diffuser with essential oils is easy to add to any room. You can also apply an essential oil to a cotton ball in a small bowl on the nightstand or common area. Aromas that are calming include lavender, rosemary, rose, ylang-ylang, chamomile, blue tansy, frankincense, jasmine, vanilla and cinnamon. Try one scent at a time to determine which ones may be effective for your loved one. If your senior is amendable to touch, a foot or hand massage, perhaps combine with a warm water soak, can be helpful. Some people enjoy having their heads or scalp rubbed. Even simply holding their hands can ground and support them during this confusing time. ( AARP )
By Hibu Websites
•
December 26, 2024
There are over 100 variants of arthritis, including osteoarthritis, rheumatoid arthritis, gout, lupus, scleroderma, and anklylosing spondylitis. Arthritis is any condition which causes swelling of one or more joints, causing stiffness and pain. Often the conditions worsen with age but are not specifically age-related. The most common and well-known types of arthritis are osteo and rheumatoid. Osteoarthritis involves damage to the cartilage on a joint. As the cartilage wears down, the bones end up grinding against one another causing pain and restricted movement. Rheumatoid Arthritis is an auto-immune condition which is an attack by the body’s immune system on the linings of the joint capsule (a membrane that encloses all the joint parts). It initially causes inflammation but eventually can destroy cartilage and bone within the joints. About 75% of rheumatoid arthritis sufferers are women. Diet and Rheumatoid Arthritis Red meat, sugar, alcohol, fat, salt, caffeine, dairy, and nightshade plants (tomatoes, potatoes, and peppers) can worsen the condition. Early clinical trials have shown that a low-fat plant-based diet has improved the condition after just a month. High fiber diets can lower the risk for knee osteoarthritis. ( Physician’s Committee for Responsible Medicine ) The most common signs of arthritis are: Pain Stiffness Swelling Redness Decreased Range of Motion The challenge can be that, for our older adults, some of these are signs of other conditions as well. Take into consideration whether your loved one also has the following risk factors: Family history – Some types of arthritis are genetic. Advanced age – Age is not a cause of arthritis but does increase the risk. Gender – Women are more likely to develop rheumatoid arthritis while men tend to develop gout or other variants. Previous joint injuries – These can increase the change of arthritis developing in that join. Obesity – Increased weight puts added stress on joints. If your loved one has other risks that would be an additional reason to pay extra attention to diet and exercise. ( John Hopkins Medicine , American College of Rheumatology and Mayo Clinic ) Treatment Arthritis has no cure. All treatments are aimed at improving quality of life. Treatments can be pharmaceutical or holistic in nature dependent on the patient’s desires. Commonly used arthritis medications include: NSAIDs are non-steroidal anti-inflammatories that are Over-The-Counter Counterirritants are creams that contain menthol or capsaicin. Steroids like prednisone reduce inflammation and can slow joint damage. They do have side effects from ongoing use and should be closely monitored by your loved one’s medical team. DMARDs (Disease-Modifying-Antirheumatic Drugs) are used with rheumatoid arthritis to slow the progression of the disease. There is an increased risk of infection with these drugs. More holistic treatments include: Exercise can increase range of motion and help with the stiffness to be expected as arthritis progresses. Close attention should be paid to the amount of pain that movements cause. Swimming and water related exercises are good alternatives. Weight loss removes pressure on aching joints. Acupuncture is used to reduce many types of pain. Glucosamine and Chondroitin have both been proven is some studies to help with arthritis pain. Fish Oil can reduce some arthritis symptoms. However, fish oil can interfere with some medications. Check with your medical team to ensure other medications are compatible. Yoga and Tai Chi are both slow moving forms of exercise that increase strength, improve mobility and help with range of motion. Find a class that is experienced with the challenges of older adults. Heat and cold can help reduce inflammation or increase mobility. Massage increase blood flow and will temporarily relive pain. Find a therapist who is knowledgeable about the pain associated with arthritis. A variety of assistive devices are available to help keep your loved one mobile. These include canes, shoe inserts, walkers, and raised toilet and chair seats. As the disease progresses, there are times when a doctor might suggest more intensive surgical measures including joint repair, joint replacement (most often hips and knees), and joint fusion (most often wrist, ankle and fingers). ( Johns Hopkins Medicine , American College of Rhematology and Mayo Clinic ) Exercise and Arthritis Exercise can help with weight loss as well as mobility. Some exercises that your loved one might enjoy include: Water walking Water aerobics Swimming Bocce ball Golf Shuffleboard Walking outdoors or on a treadmill Pilates, Tai Chi or yoga ( Arthritis Foundation )

By Hibu Websites
•
December 12, 2024
Pneumonia is an infection that inflames the air sacs on one or both lungs and may cause them to fill with fluid. It is caused by a variety of sources including bacteria, viruses, and fungi. Many of the germs that can cause pneumonia are airborne. While our bodies are generally efficient at blocking these germs; stress, lack of sleep, general depression, colds, or any weakness can allow them to sneak in. Pneumonia is the most serious for infants, people older than 65, and people with existing health challenges or weakened immune systems. It is particularly dangerous for people with heart failure or chronic lung problems. Types of Pneumonia Bacterial Pneumonia The most common form of bacterial pneumonia is pneumococcal pneumonia. Often it occurs after one has had the cold or flu. It is contagious initially but is no longer contagious after a couple days of antibiotics. Mycoplasma pneumoniae, or walking pneumonia, is a milder form of pneumonia. It is contagious and airborne. Those diagnosed often don't feel ill and are generally not hospitalized but can spread the pneumonia to others. Viral Pneumonia Viruses, including COVID-19, can cause viral pneumonia. The flu is the most common viral gateway for pneumonia. Symptoms of viral pneumonia are initially similar to those of the flu but quickly affect the lungs and breathing. Most virus generally spark only a mild form of pneumonia in health individuals. However, COVID-19 has shown that, because of its inherent propensity for lung damage, it can introduce a more severe bout with pneumonia. Older adults and people with serious illness or weak immune systems, ironically, may have fewer and milder symptoms, including a lower temperature rather than a fever. Mental acuity can be affected by a loss of oxygen to the brain, so any sudden change in mental awareness should be a cause for alarm. Fungal pneumonia Pneumonia caused by fungi is most common in people with compromised health. It is acquired through the soil or bird droppings. Ask your doctor if there are pneumonia-causing fungi in your area. ( Mayo Clinic and American Lung Association ) Symptoms of Pneumonia Chest pain when breathing or coughing Confusion or changes in mental awareness (in adults age 65 and older) Cough, which may produce phlegm Fatigue Nausea, vomiting or diarrhea Fever over 102°, sweating and shaking chills Lower than normal body temperature (in adults older than age 65 and people with weak immune systems) Bluish lips and nailbeds Shortness of breath ( Mayo Clinic ) Prevention Get vaccinated - Talk with your doctor about which might be best for your loved one. Some of the vaccines that can help include: Haemophilus influenzae type b (Hib) Influenza (flu) Measles Pertussis (whooping cough) Pneumococcal polysaccharide (recommended by the CDC for all adults over 65) Pneumococcal conjugate (recommended by the CDC for immune compromised individuals) Varicella (chickenpox) Practice good hygiene - Make sure that your loved one is washing hands and sanitizing surfaces adequately, even in their own home. Keep your immune system strong - Get enough sleep, move or exercise regularly, and eat a healthy diet. Stay away from sick people - The distancing we've all been doing is helpful but if someone in the home is sick, isolate your immuno-compromised loved ones as well. Don't smoke ( Mayo Clinic and Center for Disease Control ) Risk Factors Chronic Disease - Asthma, COPD (chronic obstructive pulmonary disease), or heart disease are primary risks. Smoking - On top of weakening the lungs, smoking generally weakens your body's natural defenses against bacteria and viruses that cause pneumonia. Compromised Immune Systems - People who have HIV/AIDS, or who have had a transplant, chemotherapy, or steroids should be aware of the risks for pneumonia. Being Hospitalized - ICU stays, especially on a ventilator, can be risky. That is not to say avoid going to the hospital if you need medical attention. Catching and treating illnesses early can help prevent a hospital stay. ( Mayo Clinic )

By Hibu Websites
•
November 28, 2024
A good first step towards taking your loved one on a longer trip is to plan a day outing or stay-cation (overnight in your own city). Some things to take into consideration: Plan the day with ample time to allow your loved one to decompress from each activity All time for a nap, if necessary Choose locations that are quieter, with fewer people, and less waiting time. Make sure that restrooms can accommodate any limitations. Start your outing at a calmer part of the day for your loved one. Let people know about your older adult by creating business sized cards to hand to clerks or restaurant staff. They can say something like “My family member has dementia. We are giving them a fun outing but they might say or do things that are unexpected. Thank you for your understanding.” Be ready to change your plans if your loved one seems to be agitated. It is not a failure on anyone’s part if your loved one can’t handle what you’ve planned. Kudos to you for trying to give them some normalcy or fun. ( National Institute of Health ) Prepare your Family Members Before a Visit Your extended family will be excited to see their loved one but may not know how to interact. Here are some easy guidelines: Keep greetings and interactions calm. Don’t speak to your loved one as if they are a child. Respect personal space and ask permission for hugs and touch. Make eye contact and call the person by name. Don’t argue if the person seems confused. Change the subject instead. Prepare to have an activity to share – a photo album, simple game, music or a walk outside. ( Daily Caring ) If you feel that your loved one can handle an extended trip, use what you’ve learned from your day trips in planning for your extended time. Before the trip Talk with your medical team to determine if there are medications that can calm them during th travel days. Be prepared to use these only, if necessary, since a sleepy traveler can make changing planes or moving from place to place more difficult. Take advantage of available assistance at the bus terminal, train station, or airport. Bring snacks that your senior likes so that you are not reliant on restaurants or airline foods. Make sure to bring important documents including insurance information, doctors’ names and phone numbers, medication lists, and medical records. Pack items for your loved one that are familiar to them and that they like holding for comfort. If they don’t have something, get them a gift of a sensory blanket, soft stuffed toy or fidget game several weeks prior to the trip to see if any of those help calm them in difficult times. Get an ID bracelet that is difficult for them to remove in case they wander off. Ensure that you have a current photo. If you are going to visit family, spend a little time beforehand looking through photo albums and talking about the people in those albums. Once you arrive at your destination Give them the opportunity to rest in a quiet location with familiar faces. Even if you are visiting family, they may not immediately feel comfortable with people they haven’t seen in a while. Plan activities that can be stepped out of easily, if necessary. Pre-identify restroom locations. Try to keep the sleep and food schedules similar to their schedules at home. ( National Institute of Health and Special Needs Alliance ) It’s OK Not to Bring Your Loved One At the end of the day, if you are planning this trip because you would like to see family and are unsure if it’s something your loved one will enjoy, reconsider whether they need to join you. Sometimes the kindest thing you can do is to leave them in the comfort of their own home with a caregiver they trust, while you take the break that you’ve earned. If you are concerned that they’ll be missing an important family gathering such as a wedding, graduation, or reunion, they can be included through video chat without the stress of travel and larger gatherings. ( Daily Caring )
Hi. Do you need any help?
VISIT US
,
This is a placeholder for the Yext Knolwedge Tags. This message will not appear on the live site, but only within the editor. The Yext Knowledge Tags are successfully installed and will be added to the website.
This is a placeholder for the Yext Knolwedge Tags. This message will not appear on the live site, but only within the editor. The Yext Knowledge Tags are successfully installed and will be added to the website.
MAILING ADDRESS
121 Progress Ave
Suite 340
Pottsville, PA 17901
HOURS
This is a placeholder for the Yext Knolwedge Tags. This message will not appear on the live site, but only within the editor. The Yext Knowledge Tags are successfully installed and will be added to the website.
Monday
Tuesday
Wednesday
Thursday
Friday
Saturday
Sunday
This is a placeholder for the Yext Knolwedge Tags. This message will not appear on the live site, but only within the editor. The Yext Knowledge Tags are successfully installed and will be added to the website.
HOURS
This is a placeholder for the Yext Knolwedge Tags. This message will not appear on the live site, but only within the editor. The Yext Knowledge Tags are successfully installed and will be added to the website.
HOURS
This is a placeholder for the Yext Knolwedge Tags. This message will not appear on the live site, but only within the editor. The Yext Knowledge Tags are successfully installed and will be added to the website.
Monday
Tuesday
Wednesday
Thursday
Friday
Saturday
Sunday
This is a placeholder for the Yext Knolwedge Tags. This message will not appear on the live site, but only within the editor. The Yext Knowledge Tags are successfully installed and will be added to the website.
CONTACT US
This is a placeholder for the Yext Knolwedge Tags. This message will not appear on the live site, but only within the editor. The Yext Knowledge Tags are successfully installed and will be added to the website.
Privacy Policy
| Do Not Share My Information
| Conditions of Use
| Notice and Take Down Policy
| Website Accessibility Policy
© 2025
The content on this website is owned by us and our licensors. Do not copy any content (including images) without our consent.






Share On: